Healthcare has a strange job. It’s expected to move fast, but it can’t afford to break things. It runs on some of the most sensitive data we have. It’s regulated. It’s operationally messy. And it still has to work on Monday morning, even when staffing is stretched and budgets are tight.
That’s exactly why emerging tech in healthcare matters beyond hospitals and clinics. Healthcare is a stress test for technology. If something can survive clinical workflows, security scrutiny, and regulatory oversight, it tends to have legs elsewhere too.
What’s changed in the last couple of years isn’t the existence of these technologies. It’s the scale. It’s the policy momentum. It’s the maturity of platforms that finally make adoption realistic. And it’s the uncomfortable truth that healthcare digital transformation can’t stay optional when demand, costs, and risk are all moving in the wrong direction.

Why Emerging Tech in Healthcare Matters to Enterprise Leaders
If you’re a healthcare chief information officer (CIO) or running a platform team, the stakes are obvious. But the ripple effects are broader than healthcare information technology (IT).
Cloud providers are being forced to support higher compliance expectations and tougher resilience requirements. Cybersecurity teams are dealing with device dense environments where “patch it later” isn’t a plan. Data leaders are being asked to make interoperability real, not aspirational, because artificial intelligence (AI) in healthcare doesn’t work without clean, connected data. Compliance leaders are tracking fast moving rulebooks that now touch everything from algorithm governance to cross border data reuse.
You can see the pressure building in the market signals. US digital health startups raised $14.2 billion in 2025, which Rock Health describes as a meaningful increase year on year and a sign that investors are treating digital health less like a novelty and more like infrastructure.
You can also see it in the “boring but important” layer: reimbursement and integration. IQVIA notes that in the United States, there are now over 300 billing codes supporting digital health tools and digital care, including 117 for software based technologies. That doesn’t mean every tool gets paid for. It does mean policymakers and payers are building a path for software to live inside real care models.
Taken together, these signals explain why the top 10 below aren’t just interesting healthcare trends. They’re technologies that are reshaping data, infrastructure, governance, and operating models under one of the strictest sets of constraints any industry has.
The Top 10 Emerging Technologies in Healthcare
Before the list, one grounding point. “Emerging” doesn’t mean experimental. It means the adoption curve is bending. The technology is becoming operational, budgetable, and harder to ignore.
1. Generative AI for Clinical and Operational Workflows
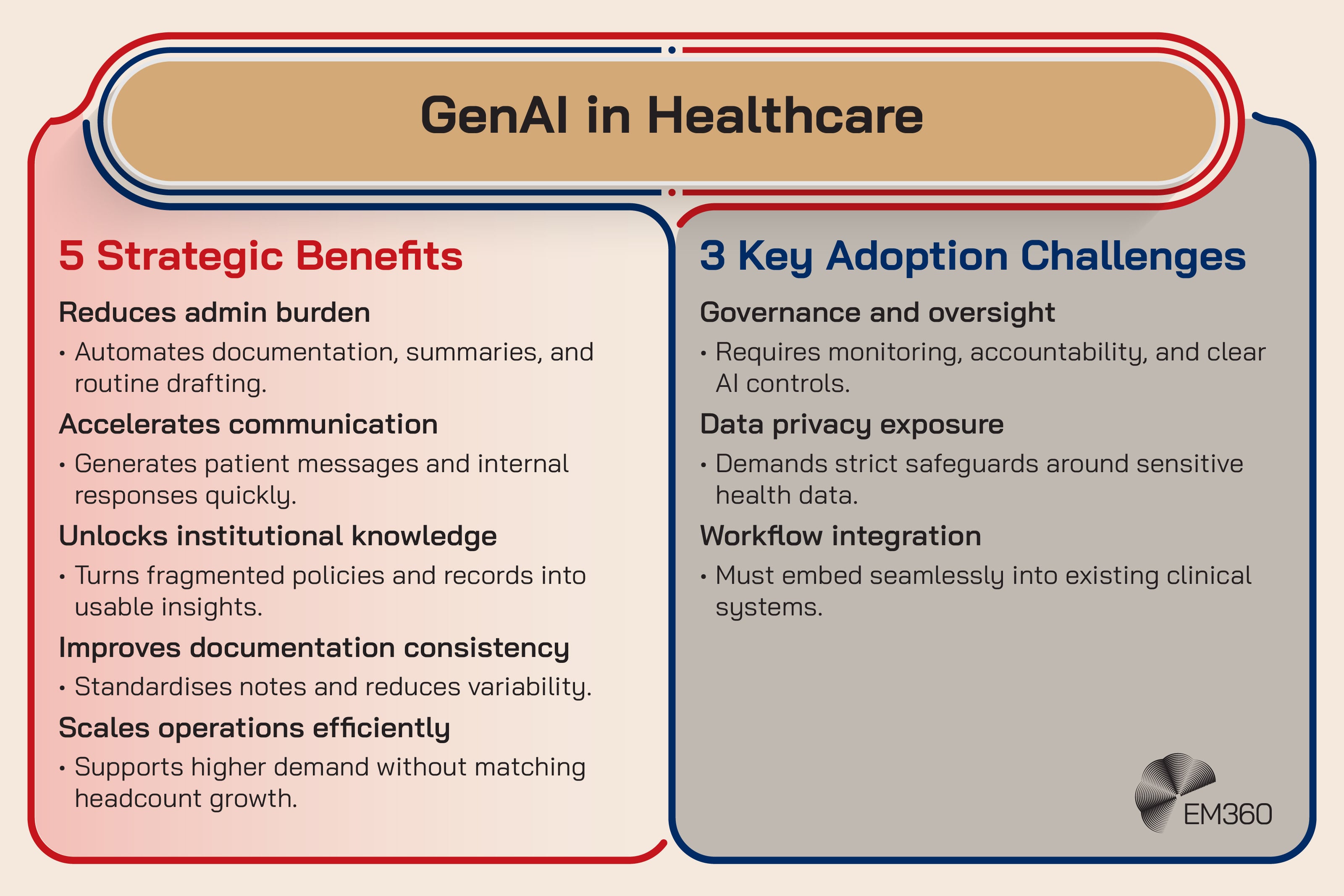
Generative AI in healthcare is the use of large language models (LLMs) to generate and summarise text, interpret requests, and automate parts of knowledge work. In practice, that shows up in clinical documentation support, referral and inbox triage, patient messaging, prior authorisation drafting, and internal search across policies and care pathways.
It’s emerging now because the models got better at language, but also because organisations are getting more serious about where the value is. The first wins aren’t “AI diagnoses cancer”. They’re fewer admin hours, faster turnaround times, and smoother workflows that clinicians and operations teams can actually tolerate.
For enterprise healthcare technology teams, the impact is structural. You need secure access controls, audit trails, and clear boundaries around what data can be used and where outputs can go. You also need governance for model lifecycle risk, because a model that changes behaviour over time becomes a compliance problem, not just a performance question.
The Food and Drug Administration’s January 2025 draft guidance on AI enabled device software functions is a useful signal here. Regulators are focusing on risk management across the total product life cycle, not just a one time approval moment.
The friction point is trust. Not philosophical trust. Operational trust. If teams can’t verify accuracy, trace sources, and constrain outputs, adoption stalls.
Strategic takeaway: Generative AI won’t scale in healthcare without data governance that’s as disciplined as the workflow it’s meant to support.
2. Ambient AI and AI Clinical Scribes
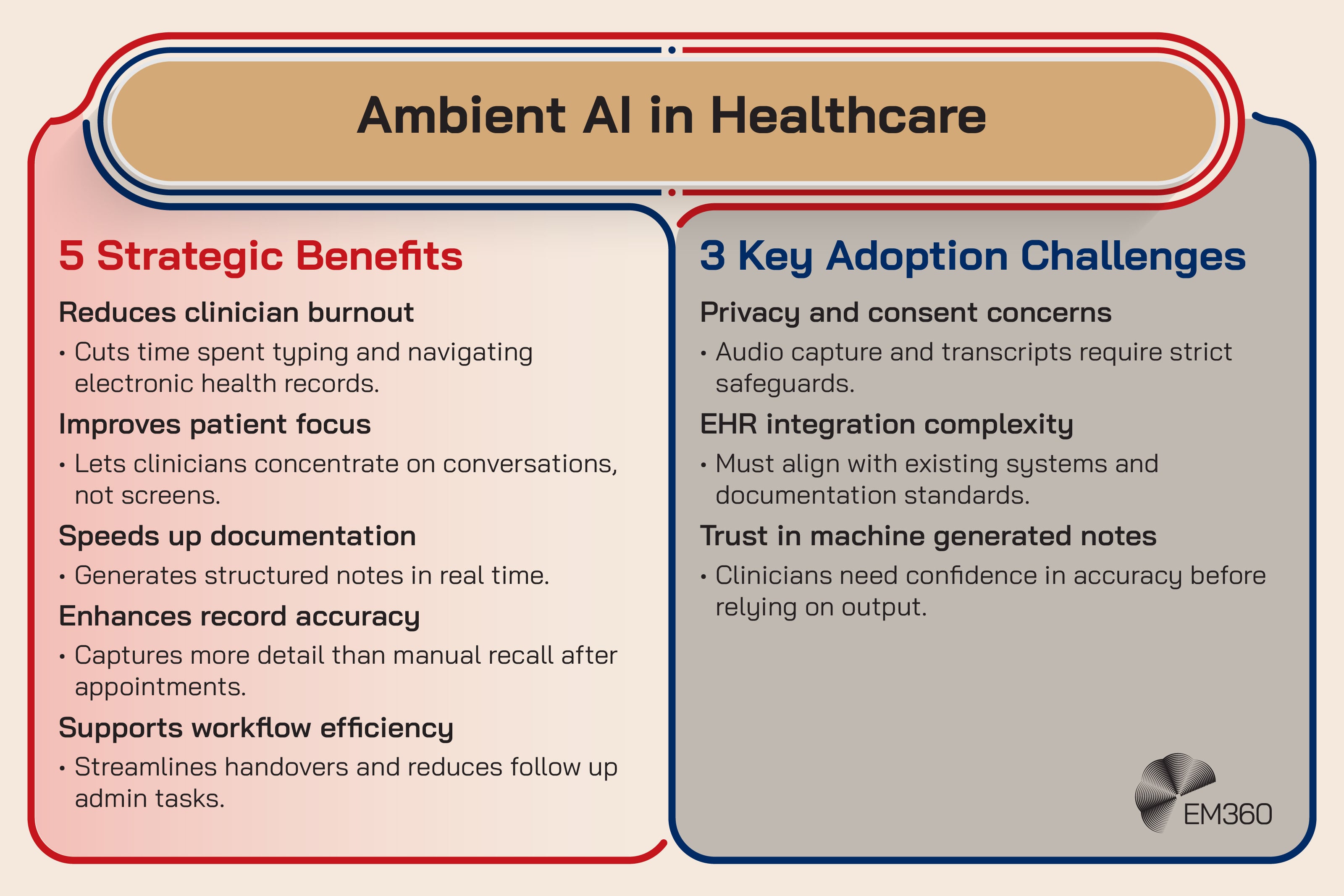
Ambient AI healthcare tools listen to clinician patient conversations and draft clinical notes automatically. The idea is simple: reduce time spent typing and clicking, and give clinicians back attention and energy.
It’s emerging now because speech recognition matured, language models improved, and health systems are reaching a breaking point on documentation burden. Unlike many AI categories, this one has a clear “pain to value” line. Less admin work is a direct operational win.
The enterprise impact sits in integration and control. These tools have to work inside electronic health records (EHRs), not alongside them. They also create new data flows. Audio is sensitive. Transcripts are sensitive. Prompts and outputs can become sensitive. That means privacy controls, retention rules, and vendor risk management all matter as much as the model quality.
The friction point is that workflow change is still change. Clinicians won’t accept a tool that adds steps, creates weird note formats, or forces them to become editors of machine output all day.
Strategic takeaway: Ambient AI succeeds when it disappears into the workflow, and fails when it turns clinicians into proofreaders.
3. AI Enabled Medical Imaging and Diagnostics
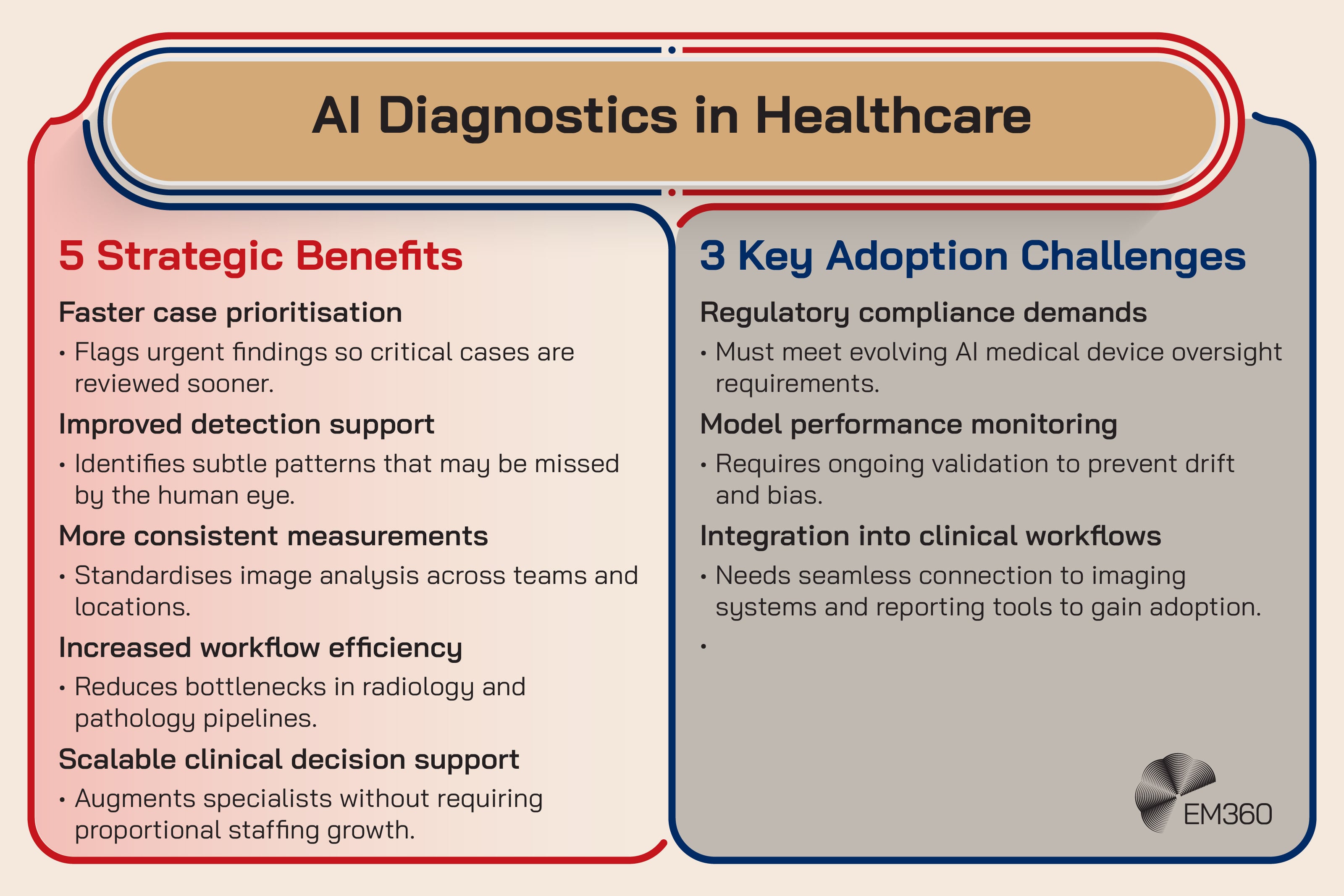
AI diagnostics use machine learning to support tasks like image triage, anomaly detection, measurement, and decision support in areas such as radiology, pathology, and cardiology. In the best cases, it helps clinicians prioritise urgent cases, reduce missed findings, and standardise measurements.
It’s emerging now because the clinical use cases are narrower and easier to validate than many other AI ambitions. Imaging and diagnostics also sit closer to established regulatory pathways, which reduces uncertainty for buyers.
The enterprise impact is governance at scale. These systems need continuous performance monitoring, because models can drift when patient populations shift, scanners change, or workflows evolve. Bias and false positives are not abstract risks. They’re operational risks that can affect clinical decisions and trust. That’s why lifecycle expectations matter, and why regulatory focus on risk management and documentation across the product life cycle is becoming central.
The friction point is procurement reality. AI imaging tools still have to justify themselves against budget constraints and integration complexity. A clinically impressive tool that can’t integrate smoothly tends to die in committee.
Strategic takeaway: AI imaging isn’t just a model problem. It’s a lifecycle monitoring and integration problem.
4. Virtual Wards and Hospital at Home Models
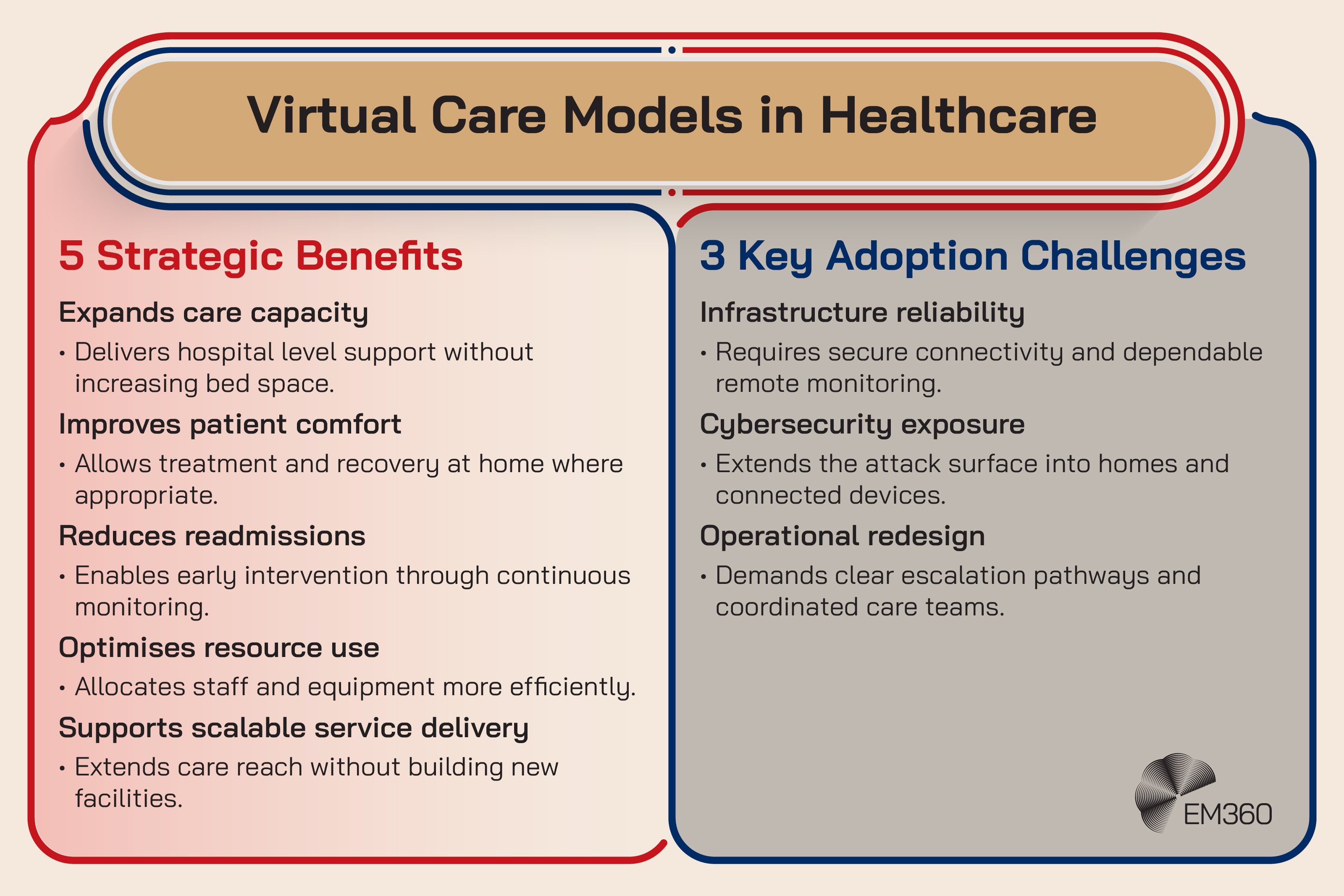
Virtual wards and hospital at home programs extend hospital grade monitoring and support into a patient’s home. This goes beyond video calls. It includes remote monitoring, escalation protocols, and coordinated teams that can intervene early.
It’s emerging now because care demand keeps rising while capacity constraints keep tightening. Health systems are also getting more experienced with hybrid care delivery models. The technology stack is catching up to the ambition, especially around connected devices and coordination tools.
The enterprise impact is that remote care is infrastructure heavy. You need reliable connectivity, secure device management, clear identity and access control, and operational analytics that help teams decide when to intervene. It also reshapes cyber risk. The attack surface extends into homes, third party devices, and more varied networks.
The friction point is operational design. Remote care programs succeed when they’re built like a service, with clear thresholds and response roles. They struggle when they’re treated like “telehealth plus gadgets”.
Strategic takeaway: Virtual wards are a care model shift first, and a technology project second.
5. Remote Patient Monitoring and Advanced Wearables
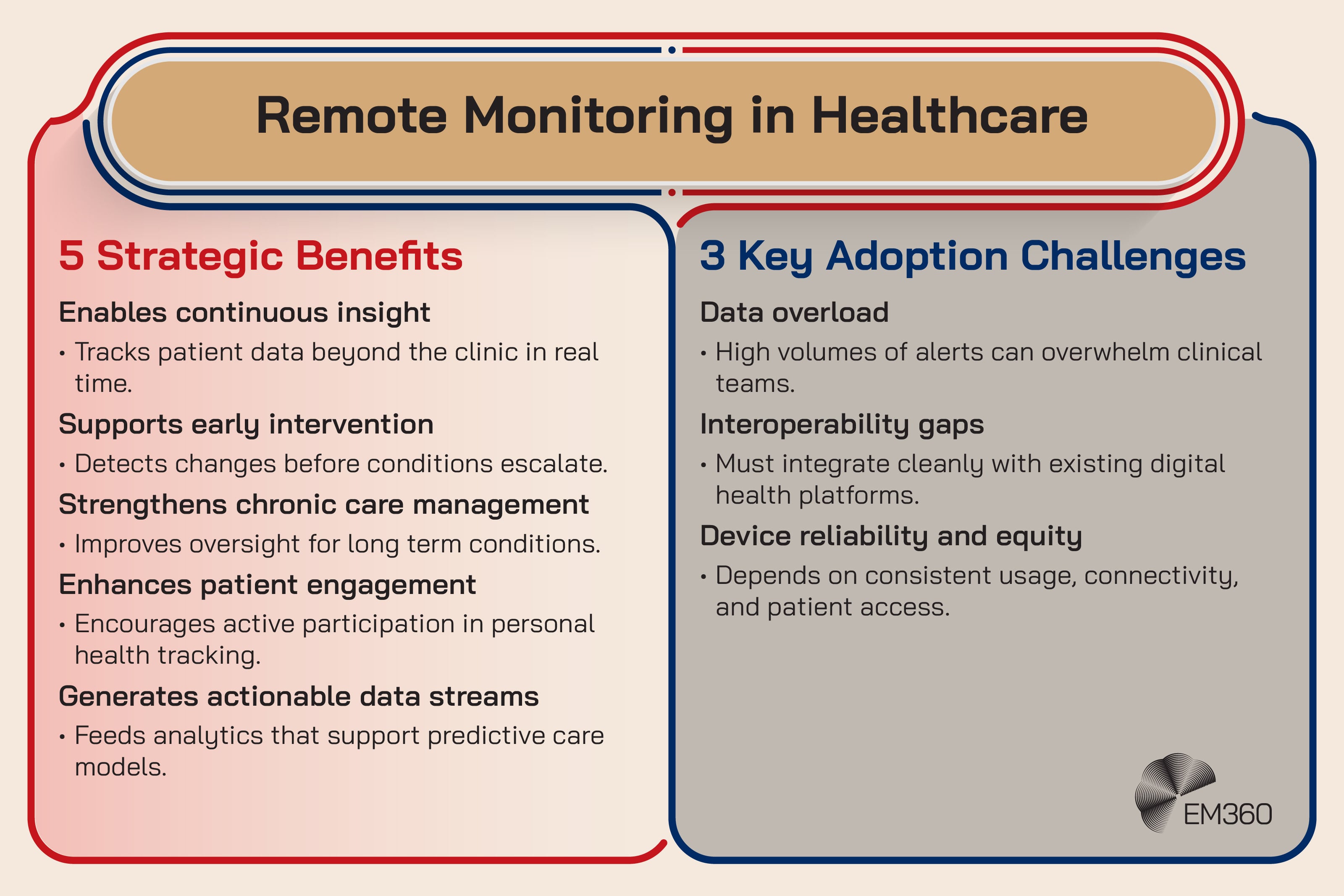
Remote patient monitoring (RPM) tracks health signals outside clinical settings, using devices that capture metrics like heart rate, oxygen saturation, glucose, or activity. Advanced wearables are pushing RPM toward continuous monitoring and more proactive interventions.
It’s emerging now because sensors are improving, consumer devices are becoming more capable, and there’s growing interest in prevention and chronic care optimisation. Payers and policymakers are also building more support for digital care models, even if the details remain messy.
The enterprise impact is data volume and signal quality. Continuous monitoring creates streams of data that can overwhelm teams if there’s no triage logic. It also raises interoperability demands. If RPM data can’t flow into EHRs and clinical workflows, it becomes a dashboard nobody checks.
The friction point is that RPM can create noise. False alarms burn staff time. Data that isn’t clinically actionable becomes a liability.
Strategic takeaway: RPM only becomes valuable when the data is connected to decisions, not just collected.
6. Internet of Medical Things and Connected Devices
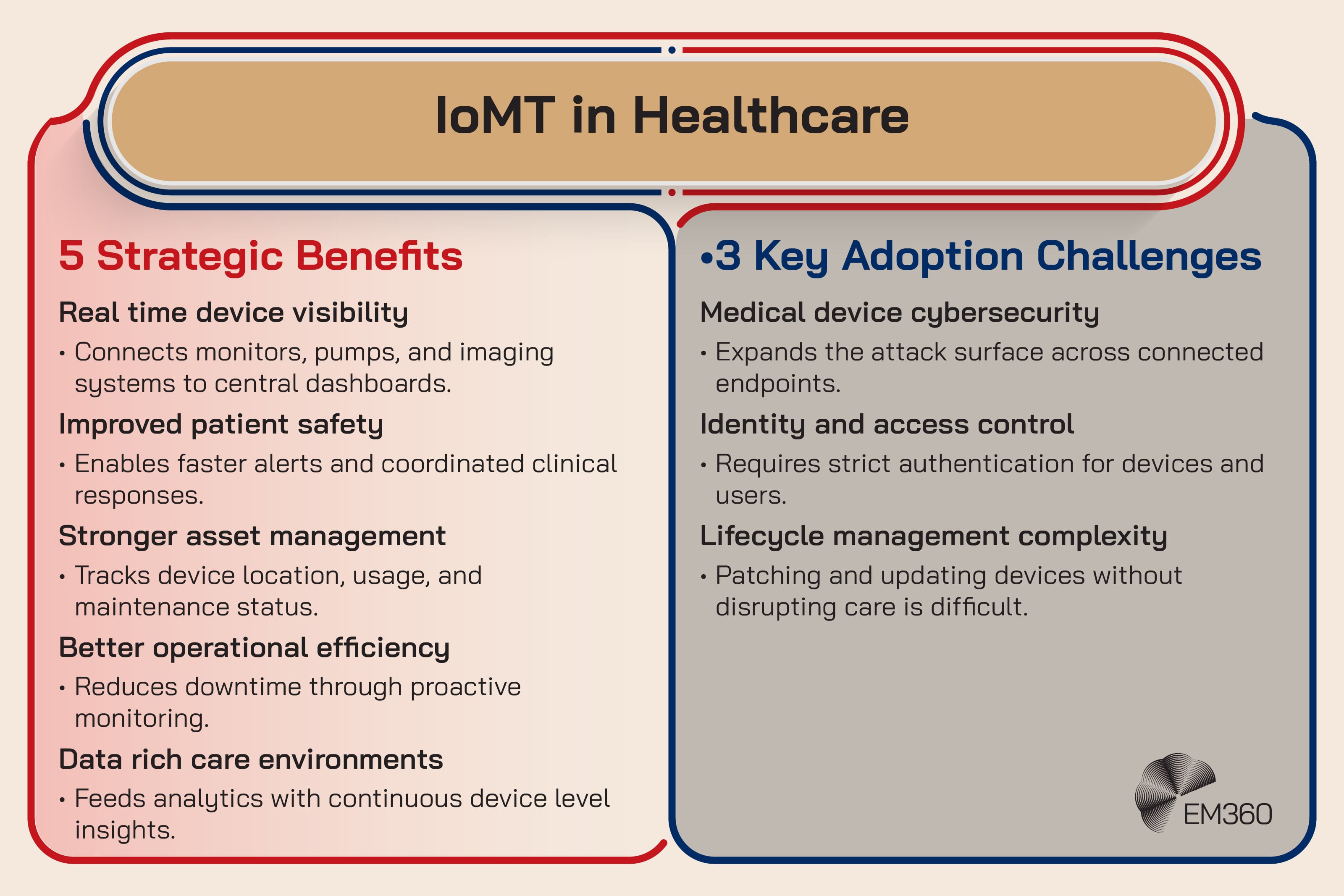
The Internet of Medical Things (IoMT) refers to network connected medical devices, from bedside monitors and infusion pumps to imaging systems and connected home devices. These devices are increasingly part of the core technology environment, not edge accessories.
It’s emerging now because device connectivity is accelerating, and because healthcare is modernising legacy estates that were never designed for today’s threat landscape. More connectivity supports better monitoring and coordination, but it also multiplies risk.
The enterprise impact is identity and security. Devices need to be inventoried, authenticated, segmented, and monitored. Patching and lifecycle management become complex when downtime isn’t acceptable. Risk management also has to account for third party dependencies, because many devices rely on vendor software stacks and remote support channels.
The friction point is that device ecosystems are hard to standardise. You end up with varied vendors, varied update cycles, and varied visibility.
Strategic takeaway: IoMT turns cybersecurity into patient safety work, whether teams like that framing or not.
7. Interoperability Platforms and Health Data Exchange
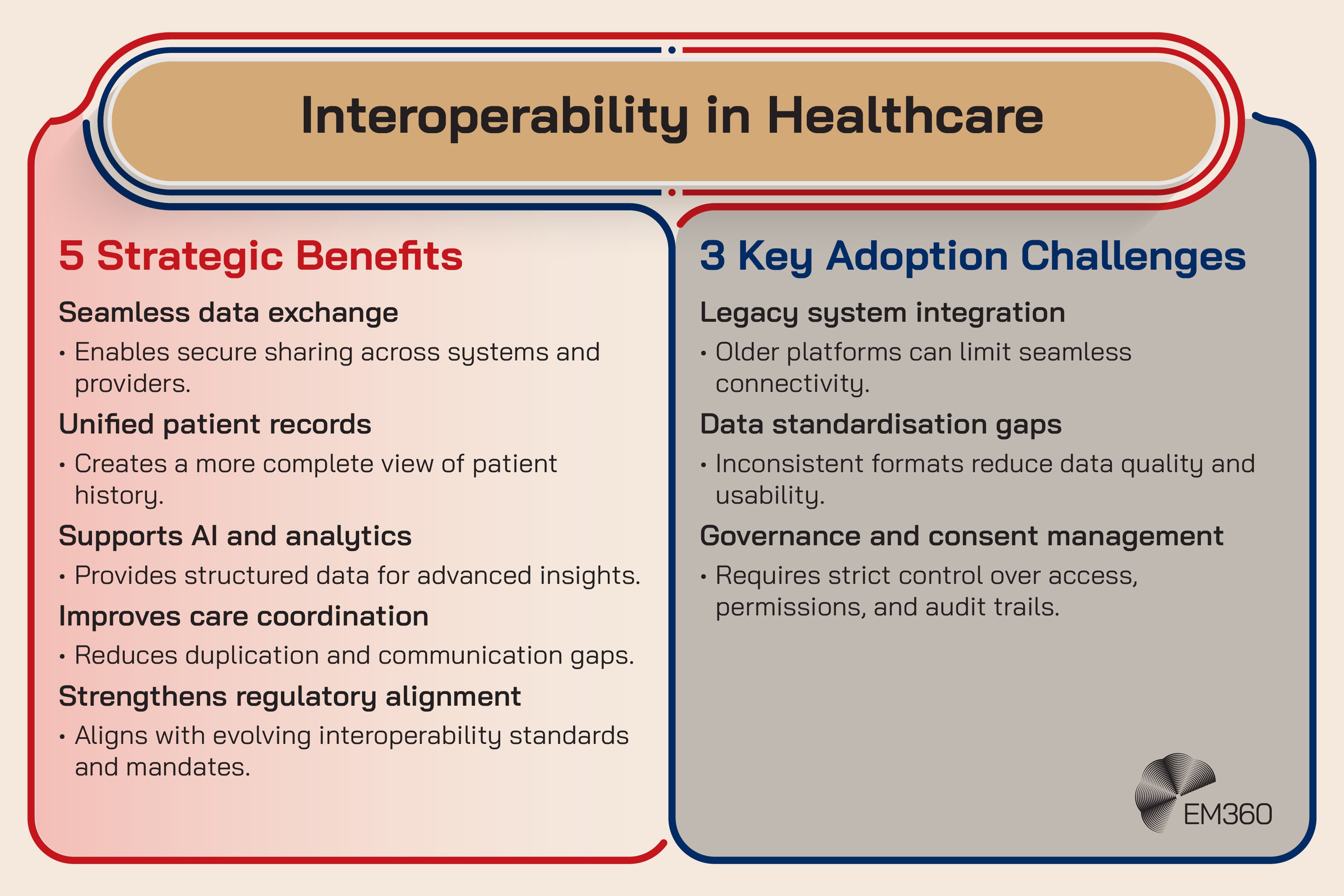
Healthcare interoperability is the ability for systems to exchange and use health data reliably, often through standards such as Fast Healthcare Interoperability Resources (FHIR) application programming interfaces (APIs). In plain terms, it’s how data moves cleanly between systems, teams, and organisations.
It’s emerging now because policy and market forces are finally converging. In Europe, the European Health Data Space (EHDS) is designed to support cross border access and sharing of electronic health data for care delivery, while also enabling secure reuse for research, innovation, policymaking, and regulatory activities. When regulation starts describing the architecture, “data liquidity” stops being a buzzword.
The enterprise impact is platform design. Organisations need data exchange layers that handle permissions, auditing, standard formats, and identity. Interoperability also shapes everything else on this list, because AI and analytics can’t scale without connected, governed data.
The friction point is implementation. Standards help, but they don’t remove the reality of legacy systems, incomplete data, and inconsistent processes.
Strategic takeaway: Interoperability is the foundation layer that makes every other healthcare innovation either possible or pointless.
8. Privacy Enhancing Technologies for Health Data
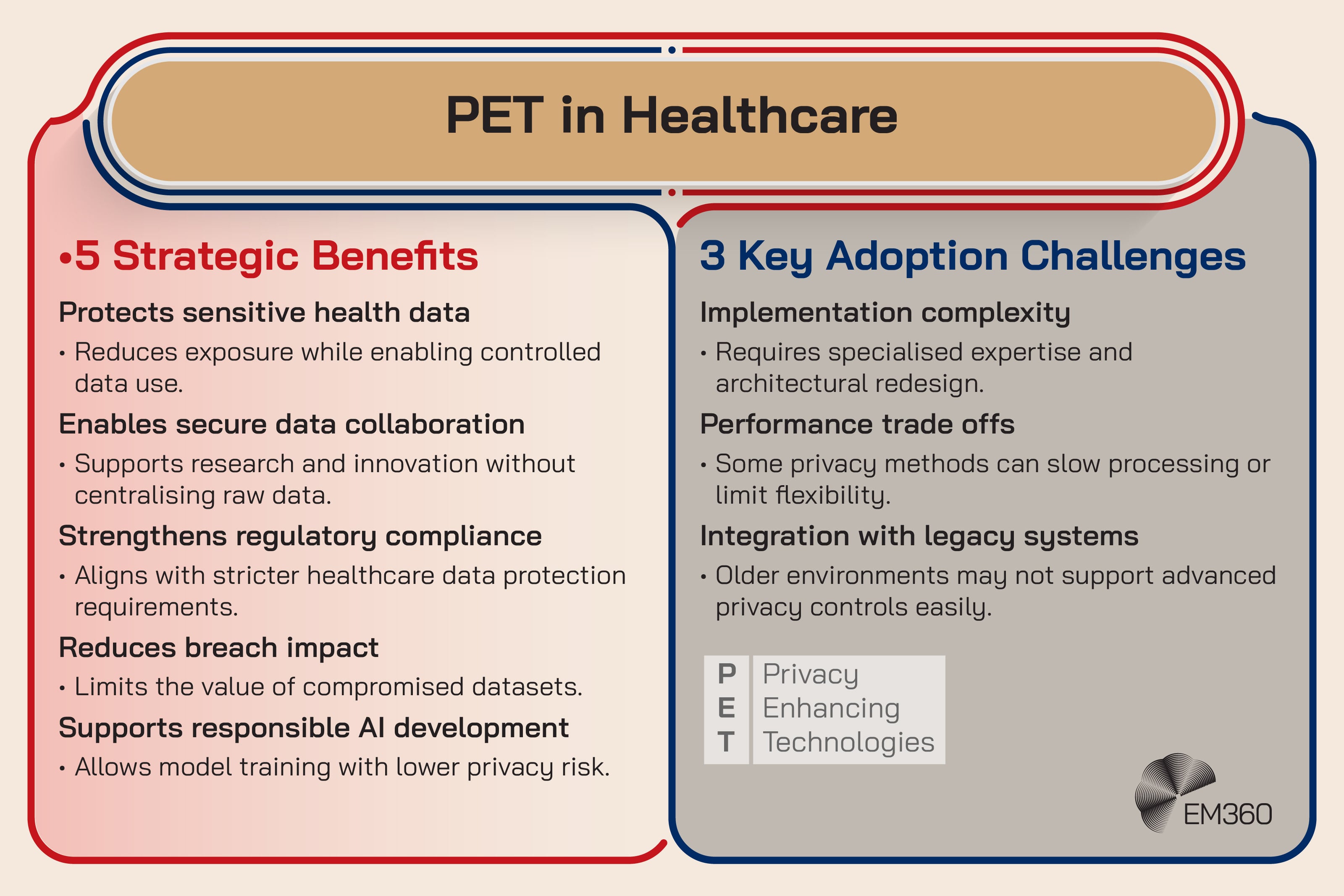
Privacy enhancing technologies (PETs) are techniques that reduce privacy and security risk while still enabling data use. In healthcare, that can include approaches like tokenisation, advanced de identification methods, secure enclaves, and federated learning, where models learn from data without centralising it.
It’s emerging now because AI and secondary data use are accelerating, and governance expectations are rising at the same time. Organisations want to use data for innovation and research, but they’re also under pressure to protect individual rights and reduce breach impact. EHDS explicitly points to secure and trustworthy reuse of health data for secondary use cases, which increases the demand for privacy preserving methods.
The enterprise impact is that privacy becomes part of architecture, not just policy. PETs can change how data is stored, processed, shared, and audited. They can also enable partnerships that would otherwise be too risky.
The friction point is complexity. PETs can be difficult to implement, and they can introduce performance or operational trade offs.
Strategic takeaway: PETs are how healthcare scales data use without scaling risk at the same rate.
9. Digital Twins for Clinical and Operational Decisions
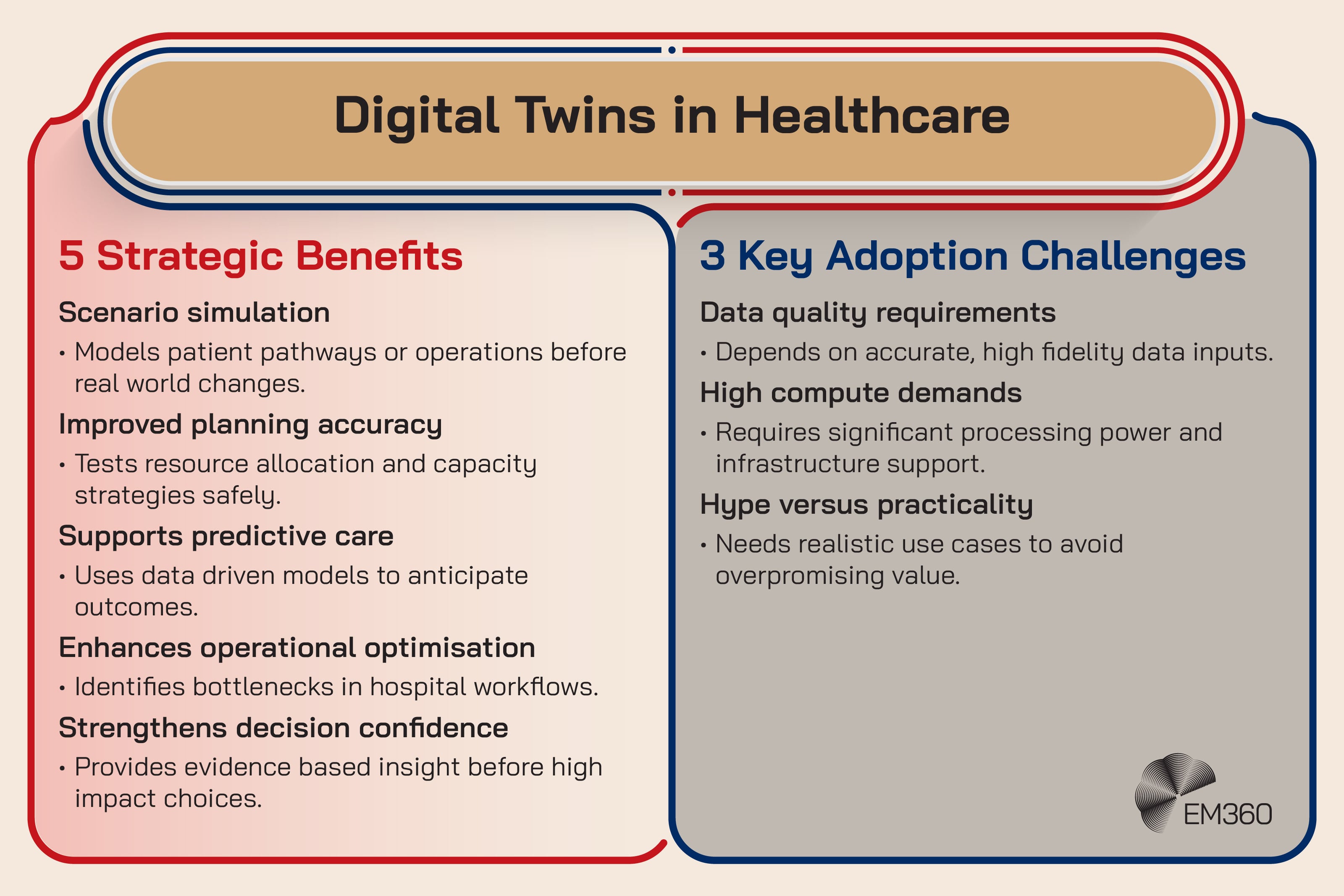
A healthcare digital twin is a digital model of something real, such as a patient, an organ system, a device, or even a hospital workflow. The goal is to simulate scenarios, predict outcomes, and test interventions safely.
It’s emerging now because data availability is improving, simulation tools are more accessible, and AI can support more sophisticated modelling. But the practical wins are still grounded. Operational twins that simulate patient flow or resource use are often more achievable than full patient level twins in the near term.
The enterprise impact is compute and data quality. Digital twins need reliable, high fidelity data. They also need serious processing capabilities, especially if simulations are meant to support time sensitive decisions.
The friction point is hype risk. When digital twins are marketed as magical replicas of humans, trust erodes. When they’re positioned as disciplined simulation tools, they’re easier to adopt.
Strategic takeaway: Digital twins are most useful when they’re treated as decision simulators, not digital clones.
10. Robotics and Intelligent Automation in Care Delivery
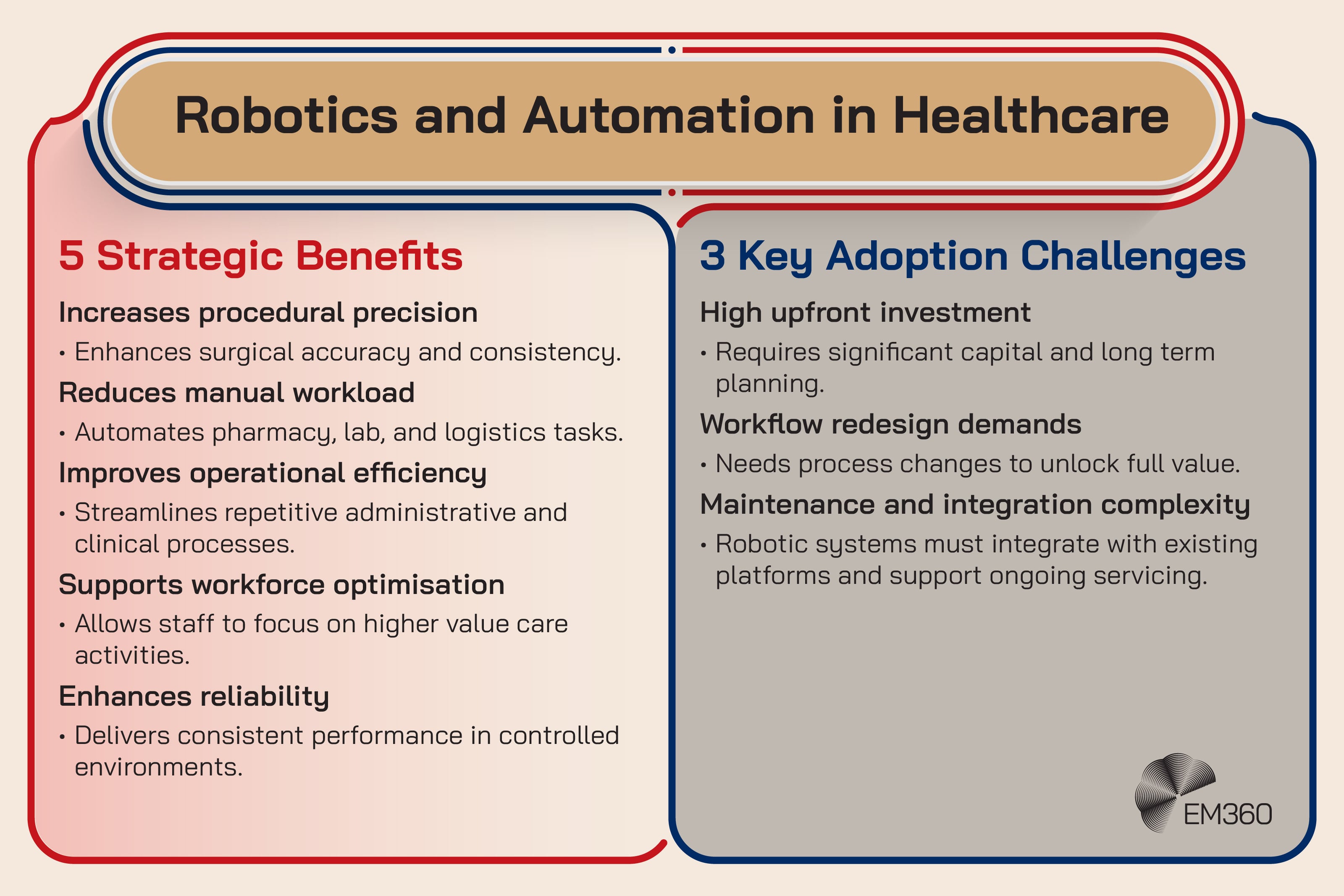
Healthcare robotics ranges from surgical robotics to pharmacy automation, lab robotics, and hospital logistics. Intelligent automation adds software driven process automation across scheduling, supply chain tasks, and administrative workflows.
It’s emerging now because robotics is moving from isolated deployments to more integrated operational systems. When robotics connects to analytics, inventory systems, and workflow orchestration, it starts delivering enterprise level productivity improvements rather than one off efficiency gains.
The enterprise impact is integration, workforce design, and reliability engineering. Robots aren’t useful if they live in a silo. They need to fit into processes, reporting, maintenance models, and safety controls. They also raise interesting governance questions, especially as AI capabilities are layered into robotic systems.
The friction point is cost and change management. Robotics projects can fail when organisations underestimate the operational redesign required to make them worthwhile.
Strategic takeaway: Robotics pays off when it’s treated as operations engineering, not equipment procurement.
What Healthcare’s Tech Acceleration Signals for the Wider Enterprise
Healthcare rarely gets to “move fast and see what happens”. That constraint creates clarity.
First, AI governance is becoming a normal operational function, not a side project. The direction of travel from regulators, including lifecycle focused expectations for AI enabled systems, is clear. The most resilient organisations are the ones treating AI risk management like any other enterprise risk, with ownership, controls, monitoring, and auditability.
Second, data architecture is being pushed by regulation, not just business ambition. EHDS is one example of how policy can force interoperability and secondary data use frameworks into the real world. That has implications for any regulated industry trying to modernise data flows without losing control.
Third, cybersecurity in device dense environments is a preview of what the broader enterprise is heading toward. As more operational technology, edge devices, and connected endpoints join networks, healthcare’s IoMT challenges start to look like a general blueprint for the next wave of enterprise security design.
Finally, the human machine workflow redesign issue isn’t going away. Tools that reduce workload and improve decision making will win. Tools that create more cognitive overhead will be quietly ignored, no matter how impressive the demo looked.
Final Thoughts: Healthcare Is Becoming the Test Bed for Enterprise Innovation
Emerging tech in healthcare isn’t a shiny list of gadgets. It’s a view into what happens when technology hits the hardest version of real life: regulated environments, fragile workflows, high consequence decisions, and data that can’t be treated casually.
After looking at these 10 technologies, the pattern is pretty consistent. The winners aren’t defined by novelty. They’re defined by whether the infrastructure is ready, whether governance is credible, and whether adoption makes life easier for the people doing the work.
Healthcare will keep being a proving ground. And the organisations paying attention now won’t just understand healthcare innovation. They’ll be better prepared for what AI, automation, connected devices, and data governance will demand across every regulated sector next.
If you want a steady way to track that shift without wading through hype cycles, EM360Tech will keep mapping where these technologies land, what’s changing at the policy and platform layer, and what it means for enterprise leaders who don’t get the luxury of guessing.




Comments ( 0 )